Inflammatory Bowel Disease (IBD)
Inflammatory Bowel Disease (IBD) is characterized by chronic inflammation of the gastrointestinal (GI) tract. Crohn’s disease and ulcerative colitis are the two most prevalent IBD conditions, and both are likely caused by a mix of genetic and environmental factors that result in issues with the immune response (1). IBD patients have consistently displayed higher levels of proinflammatory cytokines (2) as well as nitric oxide, both of which can lead to tissue damage (3).
Extivita Therapies for IBD:
Extivita Therapies IBD Recovery:

Hyperbaric Oxygen Therapy

Neurofeedback

Supplements

Nutritional IV Therapy

Pulsed Electromagnetic Field Therapy
Listen to Bryce’s experience with Hyperbaric Oxygen Therapy to treat Ulcerative Colitis
Hyperbaric Oxygen Therapy for Inflammatory Bowel Disease:

See the page on Crohn’s Disease and the page on Ulcerative Colitis for more information.
Effects of HBOT on Inflammatory Bowel Disease:

Decreased Inflammation
Increased Stem Cell Activity

New Blood Vessel Formation
Hyperbaric oxygen therapy stimulates the formation of new blood vessels, healing injured tissues that were unable to get nutrients and oxygen.

Neurofeedback for Inflammatory Bowel Disease:
There is scientific evidence showing the intimate connection between the gut and the brain, and the effect of this shared interaction on gut and psychological well-being. Patients with IBD may benefit from integration of mind and body interventions which may help decrease triggers such as stress and anxiety (6). Neurofeedback is a type of biofeedback which may be helpful in treating symptoms of IBD by calming the nervous system.
IV Therapy for Inflammatory Bowel Disease:
Patients with IBD are at risk for nutrient deficiencies because of reduced dietary intake, inflammation, and the underlying malabsorption (7). Antioxidant depletion can result from dealing with oxidative stress from inflammation occurring in IBD (9). Myers’ cocktail is a form of nutrient therapy which contains vitamin C, magnesium, B12, B6, B5, B complex, and calcium given intravenously (through the veins) (8) . This process bypasses the digestive system and a much higher level of nutrients and antioxidants is directly delivered to your cells. Myers’ cocktail and glutathione are safe and effective adjunctive treatments for IBD.
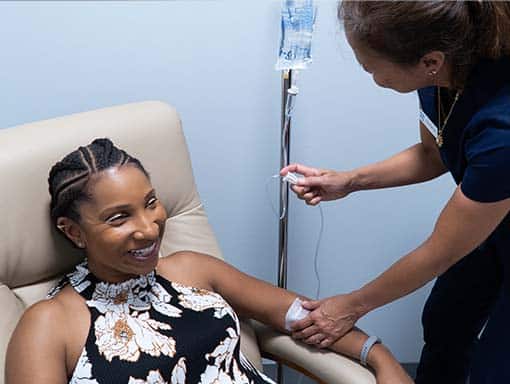

Pulsed Electromagnetic Field Therapy for IBD:
According to studies, the microcirculation and inside lining of the blood vessels play a critical role in body’s immune balance. In IBD, micro vessels in chronically inflamed and can result in decreased oxygen and nutrient delivery to tissues. In addition, micro vessels are also found to have reduced vessel diameter, vascular density, and diminished blood flow (10, 11). When used in conjunction with HBOT, PEMF therapy may lead to improved microvascular function, blood flow, and therefore tissue and organ health.
News & Research for Inflammatory Bowel Disease:
Efficacy of hyperbaric oxygen in patients with Crohn’s disease: two case reports.
Crohn’s disease is an inflammatory disease of the gastrointestinal tract, usually involving the ileum, that can lead to debilitating symptoms of abdominal pain, diarrhea and malabsorption during acute exacerbations. Because there is no known cause of the illness, treatment is based upon symptomatology and may ultimately require bowel resection if response to medical therapy is inadequate. Treatment with hyperbaric oxygen has shown promise in the reduction of inflammation associated with acute exacerbations of Crohn’s disease, with alleviation of symptoms and an improvement in quality of life. We present two cases of pediatric patients with exacerbations of Crohn’s disease who underwent cycles of hyperbaric oxygen therapy.
A favourable response to surgical intervention and hyperbaric oxygen therapy in pyoderma gangrenosum.
Pyoderma gangrenosum (PG) is a neutrophilic dermatosis characterised with ulcerations. Inflammatory bowel diseases (ulcerative colitis and Crohn’s disease) and haematologic diseases (leukaemia, preleukaemia and monoclonal gammopathy) have been reported in about 40-50% of PG patients in whom the treatment of the underlying disease is important for the improvement of the lesions. We herein report a colorectal adenocarcinoma patient with PG, who responded partially to topical treatments and systemic immunosuppressants and healed completely with the aid of surgical wound repair and hyperbaric oxygen therapy.
[Hyperbaric oxygen in the treatment of perineal Crohn’s disease era of infliximab: a renewal interest?].
Despite the growing number of therapeutic methods and the recent introduction of new drugs more active in the therapeutic arsenal, lesions of the ano-perineal Crohn’s disease remains difficult to support. Hyperbaric oxygen (HBO) was made before the era of infliximab, an interesting therapeutic approach in which the current position remains unclear. To assess HBO efficacy in the treatment of anal fistulas refractory Crohn’s disease. Literature review. Hyperbaric oxygen therapy was used in the 90’s when the biotherapy was not part of the armamentarium for Crohn’s disease. Research conducted has identified only nine publications evaluating the efficacy of hyperbaric oxygen therapy in the treatment of anal fistulas refractory Crohn’s disease.
References
- Mattos, Bruno Rafael Ramos de, Maellin Pereira Gracindo Garcia, Julia Bier Nogueira, Lisiery Negrini Paiatto, Cassia Galdino Albuquerque, Caique Lopes Souza, Luís Gustavo Romani Fernandes, Wirla Maria da Silva Cunha Tamashiro, and Patricia Ucelli Simioni. “Inflammatory Bowel Disease: An Overview of Immune Mechanisms and Biological Treatments.” Mediators of Inflammation 2015 (2015). https://doi.org/10.1155/2015/493012.
- Papadakis, K. A., and S. R. Targan. “The Role of Chemokines and Chemokine Receptors in Mucosal Inflammation.” Inflammatory Bowel Diseases 6, no. 4 (November 2000): 303–13. https://doi.org/10.1002/ibd.3780060408.
- Rachmilewitz, D., J. S. Stamler, D. Bachwich, F. Karmeli, Z. Ackerman, and D. K. Podolsky. “Enhanced Colonic Nitric Oxide Generation and Nitric Oxide Synthase Activity in Ulcerative Colitis and Crohn’s Disease.” Gut 36, no. 5 (May 1995): 718–23. https://doi.org/10.1136/gut.36.5.718.
- Akin, M. L., B. M. Gulluoglu, H. Uluutku, C. Erenoglu, E. Elbuken, S. Yildirim, and T. Celenk. “Hyperbaric Oxygen Improves Healing in Experimental Rat Colitis.” Undersea & Hyperbaric Medicine: Journal of the Undersea and Hyperbaric Medical Society, Inc 29, no. 4 (2002): 279–85. https://www.ncbi.nlm.nih.gov/pubmed/12797669
- Granowitz, E. V., E. J. Skulsky, R. M. Benson, J. Wright, J. L. Garb, E. R. Cohen, E. C. Smithline, and R. B. Brown. “Exposure to Increased Pressure or Hyperbaric Oxygen Suppresses Interferon-Gamma Secretion in Whole Blood Cultures of Healthy Humans.” Undersea & Hyperbaric Medicine: Journal of the Undersea and Hyperbaric Medical Society, Inc 29, no. 3 (2002): 216–25. https://www.ncbi.nlm.nih.gov/pubmed/12670123
- Yeh, Ann Ming et al. “Mind-Body Interventions for Pediatric Inflammatory Bowel Disease.” Children (Basel, Switzerland) vol. 4,4 22. 3 Apr. 2017, doi:10.3390/children4040022
- Waśko-Czopnik, Dorota, and Leszek Paradowski. “The influence of deficiencies of essential trace elements and vitamins on the course of Crohn’s disease.” Advances in clinical and experimental medicine : official organ Wroclaw Medical University vol. 21,1 (2012): 5-11.
- Gaby, Alan R. “Intravenous nutrient therapy: the “Myers’ cocktail“. Alternative medicine review: a journal of clinical therapeutic 7 5 (2002): 389-403.
- Yan, Haiyan et al. “Ascorbic acid ameliorates oxidative stress and inflammation in dextran sulfate sodium-induced ulcerative colitis in mice.” International journal of clinical and experimental medicine vol. 8,11 20245-53. 15 Nov. 2015
- Deban, Livija et al. “Multiple pathogenic roles of microvasculature in inflammatory bowel disease: a Jack of all trades” The American journal of pathology vol. 172,6 (2008): 1457-66. doi:10.2353/ajpath.2008.070593
- Hatoum, Ossama A et al. “The vascular contribution in the pathogenesis of inflammatory bowel disease.” American journal of physiology. Heart and circulatory physiology vol. 285,5 (2003): H1791-6. doi:10.1152/ajpheart.00552.2003
