Traumatic Brain Injury (TBI)
The treatment of TBI is critical; it is estimated that between 3.2 and 5.3 million Americans live with permanent disabilities as a direct result of a TBI(1). Traumatic brain injuries (TBI) refer to injuries to the brain caused by an external physical force(2). Such injuries result in brain dysfunction, which can lead to cognitive impairments such as decreased attention, memory loss, and reduced cognitive flexibility as well as motor issues(3). However, there is compelling evidence to suggest that HBOT may significantly reduce the negative symptoms experienced by TBI patients, even years after the incident.
Extivita Therapies for TBI:
Extivita Therapies Traumatic Brain Injury Recovery:

Hyperbaric Oxygen Therapy

Neurofeedback

Supplements

Nutritional IV Therapy

Pulsed Electromagnetic Field Therapy
Hyperbaric Oxygen Therapy for Traumatic Brain Injury:
Research suggests that increased tissue oxygenation, improved cellular metabolism and mitochondrial function, and improved inflammatory response, to name a few, are responsible for improving the following cognitive impairments(5):
- Improved Memory (most improvement)
- Reduced Attention Problems (high improvement)
- Improved Executive Function
- Increased Information Processing Speed
- Improved Motor Skills
Effects of HBOT on Traumatic Brain Injury:

Decreased Inflammation
Increased Stem Cell Activity

New Blood Vessel Formation
Hyperbaric oxygen therapy stimulates the formation of new blood vessels, healing injured tissues that were unable to get nutrients and oxygen.
Neurofeedback for Traumatic Brain Injury:
Neurofeedback has been shown to improve many of the cognitive issues that patients with traumatic brain injuries (TBIs) experience post-injury(6, 7). After a TBI, the brain must form new neural pathways to account for any brain tissue damaged by the TBI. These new connections play a vital role in restoring healthy brain function, and neurofeedback has been shown to help establish and help strengthen such connections(6). Most studies that use neurofeedback to help TBIs train to increase theta and alpha brainwaves in the occipital lobe (towards the back of the head). This has been shown to improve reduce stress (which has a negative physiological and emotional effect in TBIs), increase relaxation, and improve cognitive measures such as memory and processing speed. (6, 7, 8, 9).
IV Therapy for Traumatic Brain Injury:
The combination of the Myer’s cocktail and glutathione IV’s can improve cognitive and motor function following traumatic brain injury. A principal issue post-TBI is the degree neuroinflammation, which is directly correlated to the severity of the short-term and long-term consequences of TBI. In TBI patients, the mitochondria in brain cells become damaged, activating immune cells (glia, microglia, and astrocytes). These immune cells release inflammatory cytokines which recruit even more inflammatory cells to the area. This results in brain cell swelling, death, decreased energy production, all of which lead to impaired cognitive and motor function(10).
The Myers cocktail IV contains Vitamin C and other antioxidants which have been shown to decrease oxidative stress and inflammatory responses. By doing do, the Myer’s cocktail can help minimize further cells damage and improve brain health and function after a TBI(11, 12). Glutathione, the master antioxidant, has been used to reduce oxidative stress and enhance cellular detoxification and can be part of a multi-modal therapy in correcting the metabolic crisis in TBI.
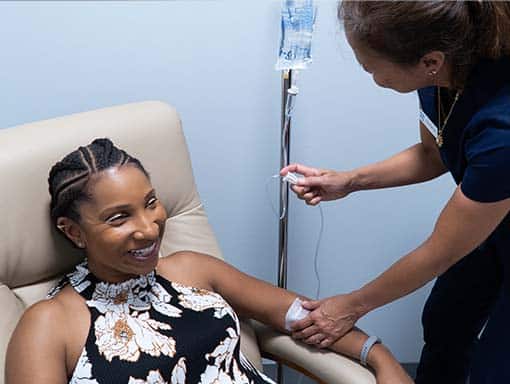
Pulsed Electromagnetic Field Therapy for Traumatic Brain Injury:
Micro vessels play a significant role in overall course of vascular diseases. Dysfunction to this system has been linked to a multitude of illnesses. The PEMF device has been shown to optimize the microcirculatory system, increasing perfusion to tissues and organs. When used in conjunction with HBOT, oxygen rich blood can be delivered to these areas, where healing can begin (13).
News & Research for for Traumatic Brain Injury:
Evidence brief: hyperbaric oxygen therapy (HBOT) for traumatic brain injury and/or post-traumatic stress disorder.
This report is a product of the VA Evidence-based Synthesis Program. The purpose is to provide “timely and accurate syntheses of targeted healthcare topics. to improve the health and healthcare of Veterans”. The authors have made a comprehensive search and analysis of the literature and make recommendations to assist clinicians in dealing with veterans suffering from either traumatic brain injury (TBI) or post-traumatic stress disorder (PTSD). The report is timely and of great potential impact given the vigorous and lengthy debate among hyperbaric physicians and lay people determined to find an answer for the large numbers of veterans deeply affected with some combination of PTSD and post-concussion dysfunction.
HYPERBARIC OXYGEN THERAPY- BASICS AND NEW APPLICATIONS
Hyperbaric oxygen therapy (HBOT) serves as primary or adjunctive therapy for a diverse range of medical conditions. The indication for HBOT can be related to either pressure (decompression sickness or air emboli) or tissue hypoxia. It is now realized, that the combined action of hyperoxia and hyperbaric pressure, leads to significant improvement in tissue oxygenation while targeting both oxygen and pressure sensitive genes, resulting in improved mitochondrial metabolism with anti-apoptotic and anti-inflammatory effects. Clinical studies published in recent year’s present convincing evidence that HBOT can be the coveted neurotherapeutic method for brain repair. Here we discuss the multi-faceted role of HBOT in wound care in general and in neurotherapeutics in detail.
Arizona Legislature Approves Hyperbaric Oxygenation Treatment for Veterans with Traumatic Brain Injury
TUCSON, Ariz., April 02, 2018 (GLOBE NEWSWIRE) -- Veterans with traumatic brain injuries (TBI) and selected post-traumatic stress disorder (PTSD) conditions would be eligible to participate in hyperbaric oxygenation therapy (HBOT) under a bill approved unanimously in...
References
- Tbi_report_to_congress_epi_and_rehab-a.Pdf.” Accessed June 2, 2019. https://www.cdc.gov/traumaticbraininjury/pdf/tbi_report_to_congress_epi_and_rehab-a.pdf.
- Silver, J.M., T.W. McAllister, and D.B. Arciniegas. Textbook of Traumatic Brain Injury. American Psychiatric Publishing, 2018. https://books.google.com/books?id=ViKMDwAAQBAJ.
- Hadanny A, Abbott S, Suzin G, et al. Effect of hyperbaric oxygen therapy on chronic neurocognitive deficits of post-traumatic brain injury patients: retrospective analysis. BMJ Open 2018;8:e023387. doi: 10.1136/bmjopen-2018-023387 https://bmjopen.bmj.com/content/bmjopen/8/9/e023387.full.pdf
- Boussi-Gross R, Golan H, Fishlev G, et al. Hyperbaric oxygen therapy can improve post concussion syndrome years after mild traumatic brain injury – randomized prospective trial. PLoS One 2013;8(11):e79995 https://www.ncbi.nlm.nih.gov/pubmed/24260334
- Efrati S, Ben-Jacob E. Reflections on the neurotherapeutic effects of hyperbaric oxygen. Expert Rev Neurother 2014;14:233–6. https://www.tandfonline.com/doi/full/10.1586/14737175.2014.884928
- Munivenkatappa, Ashok, et al. “EEG Neurofeedback Therapy: Can It Attenuate Brain Changes in TBI?” NeuroRehabilitation, vol. 35, no. 3, IOS Press, Jan. 2014, pp. 481–84. content.iospress.com, doi:10.3233/NRE-141140.
- Bennett, Cathlyn N., et al. “Clinical and Biochemical Outcomes Following EEG Neurofeedback Training in Traumatic Brain Injury in the Context of Spontaneous Recovery:” Clinical EEG and Neuroscience, SAGE PublicationsSage CA: Los Angeles, CA, Dec. 2017. Sage CA: Los Angeles, CA, journals.sagepub.com, doi:10.1177/1550059417744899.
- Reddy, Rajakumari Pampa, et al. “Silent Epidemic: The Effects of Neurofeedback on Quality-of-Life.” Indian Journal of Psychological Medicine, vol. 36, no. 1, 2014, pp. 40–44. PubMed Central, doi:10.4103/0253-7176.127246.
- Reddy, Rajakumari P., et al. “Neurofeedback Training to Enhance Learning and Memory in Patient with Traumatic Brain Injury: A Single Case Study.” The Indian Journal of Neurotrauma, vol. 6, no. 1, June 2009, pp. 87–90. ScienceDirect, doi:10.1016/S0973-0508(09)80037-3.
- Cheng, G., Kong, R.‐h., Zhang, L.‐m. and Zhang, J.‐n. (2012), Mitochondria in traumatic brain injury and mitochondrial‐targeted multipotential therapeutic strategies. British Journal of Pharmacology, 167: 699-719. doi:10.1111/j.1476-5381.2012.02025.x
- KC, Sagan et al. “Vitamin C enters mitochondria via facilitative glucose transporter 1 (Glut1) and confers mitochondrial protection against oxidative injury.” FASEB journal : official publication of the Federation of American Societies for Experimental Biology vol. 19,12 (2005): 1657-67. doi:10.1096/fj.05-4107com
- Zhang, Xiao-Ying et al. “Vitamin C alleviates LPS-induced cognitive impairment in mice by suppressing neuroinflammation and oxidative stress.” International immunopharmacology vol. 65 (2018): 438-447. doi:10.1016/j.intimp.2018.10.020
- https://www.imin-org.eu/images/science/Haug-Report-Bemer_2016_Englisch.pdf
